The MASLD Diet: What to Eat to Support Liver Health

Something feels off — low energy, a sluggish digestion, maybe a doctor’s visit that raised more questions than it answered. For many people, the liver is the last organ they think to connect to these symptoms.
If you’ve recently been told your liver is showing signs of fat accumulation, it can feel overwhelming. But this may not be random — it may signal that your metabolic health needs direct support.
The encouraging news: the MASLD diet is one of the most practical and evidence-backed tools available for improving liver health. Targeted food choices can help reduce liver fat, lower inflammation, and support your body’s own repair processes.
What Is the MASLD Diet and How Does It Support the Liver?
The MASLD diet centers on whole, anti-inflammatory foods that reduce the metabolic burden on the liver. Unlike restrictive elimination plans, it’s a pattern of eating — not a temporary fix.
Following the MASLD diet consistently may help reduce liver fat and improve key metabolic markers, sometimes within weeks of making changes. The core of this approach emphasizes fiber, antioxidants, lean protein, and healthy fats — nutrients that work together to protect liver cells and support insulin sensitivity.
| Nutrient Category | Best Food Sources | Key Liver Benefit |
|---|---|---|
| Antioxidants | Berries, leafy greens, walnuts, green tea | Reduces cellular stress and oxidative damage |
| Fiber | Oats, lentils, broccoli, apples, chia seeds | Supports blood sugar balance and weight management |
| Healthy Fats | Olive oil, avocado, salmon, sardines, almonds | May reduce harmful inflammation |
| Lean Protein | Eggs, chicken, tofu, Greek yogurt, legumes | Supports tissue repair without excess dietary fat |

Understanding MASLD and Why Food Choices Matter
MASLD — metabolic dysfunction-associated steatotic liver disease — is the updated name for what was previously called non-alcoholic fatty liver disease (NAFLD). The renaming reflects a more accurate understanding: this condition is driven by metabolic dysfunction, not alcohol. For a closer look at how the two conditions differ in cause and management, alcoholic vs. non-alcoholic fatty liver disease breaks down the key distinctions.
It’s linked to insulin resistance, high blood pressure, elevated triglycerides, and excess visceral fat — a cluster of risk factors that also defines metabolic syndrome. Roughly 1 in 4 adults globally are estimated to have some degree of liver fat accumulation — most without any clear symptoms early on.
How the Liver Is Affected Over Time
MASLD progresses in stages. Simple fat accumulation (steatosis) is the earliest and most reversible phase. Left unaddressed, it can advance to steatohepatitis — where inflammation develops — and eventually to fibrosis or cirrhosis.
The good news is that the earliest stages respond well to dietary and lifestyle changes. Research suggests that losing 5–10% of body weight through whole-food dietary shifts can measurably reduce liver fat.[4]
| Stage | What Happens | Key Note |
|---|---|---|
| Simple Steatosis | Fat collects in liver cells | Often asymptomatic; most responsive to dietary change |
| Steatohepatitis | Inflammation joins the fat | Liver cells can be injured; dietary intervention still effective |
| Fibrosis | Scar tissue begins to form | Early scarring can still be managed with lifestyle changes |
| Cirrhosis | Widespread scarring changes liver structure | Advanced stage; medical supervision essential |
The “You’re Not Alone” Reality
Many people find out about liver fat incidentally — on a routine scan or after slightly elevated liver enzymes show up in bloodwork. Understanding what those numbers actually mean is an important first step; what liver enzyme results actually mean explains ALT, AST, ALP, and GGT in plain language.
This condition often develops quietly over years, shaped by insulin resistance, sleep patterns, and dietary habits — not by any single failure. It is not a personal shortcoming, and it is far more common than most people realize.
Best Foods for the MASLD Diet
The MASLD diet isn’t about restriction — it’s about crowding out the foods that burden the liver with ones that actively support it. Specificity matters here more than general advice about “eating healthy.”
Vegetables and Fiber-Rich Foods
Leafy greens, broccoli, Brussels sprouts, zucchini, and peppers are especially valuable. They’re low in calories, high in fiber, and rich in compounds that support liver detoxification pathways.
Aim to fill at least half your plate with vegetables at each meal. This isn’t just a general wellness tip — fiber intake is directly linked to lower fasting insulin and reduced hepatic fat accumulation.[1]
Healthy Fats and Omega-3 Sources
Extra virgin olive oil is one of the most studied foods in liver health research. Regular use is associated with reduced liver enzyme levels and lower hepatic inflammation.
Fatty fish — salmon, sardines, mackerel — provide omega-3 fatty acids that may directly reduce liver triglycerides. Research suggests two to three servings per week is a reasonable target for those managing liver fat.[3]
Protein Sources That Support Liver Function
Eggs, Greek yogurt, legumes (lentils, chickpeas, black beans), and tofu provide lean protein without the saturated fat load of processed meats.
Legumes deserve special mention: their combination of plant protein and soluble fiber appears to slow gastric emptying and blunt post-meal glucose spikes — two mechanisms directly relevant to reducing liver fat.[1]
What to Limit or Avoid
- Added sugars and sugar-sweetened beverages — fructose is processed almost entirely in the liver and contributes directly to de novo lipogenesis (fat production)
- Refined carbohydrates: white bread, white rice, pastries, crackers
- Processed and ultra-processed foods high in trans fats or seed oils
- Red and processed meats in excess — associated with higher liver inflammation markers
- Alcohol — even moderate intake can accelerate liver fat progression in those with MASLD
For a comprehensive breakdown of which specific foods have the strongest evidence behind them, the best foods for liver health goes deeper on individual choices and the research supporting them.

Evidence-Based Dietary Patterns for Liver Health
Several structured eating patterns have been studied directly in people with fatty liver disease. They’re not interchangeable — each has strengths depending on individual health context.
The Mediterranean Diet: Strongest Liver Evidence
The Mediterranean pattern has the most robust evidence base for MASLD specifically. A large study of 3,325 adults found that high adherence was associated with a 32% lower risk of advanced liver fibrosis.[2]
A practical starting point: grilled salmon over a quinoa salad with olive oil and roasted vegetables. Or a lentil soup with crusty whole-grain bread and a side of leafy greens. The pattern prioritizes plants, fish, olive oil, and legumes — with red meat and processed foods as occasional exceptions.
DASH and Plant-Based Approaches
The DASH diet has shown benefit in clinical trials for people with liver disease who also have high blood pressure or type 2 diabetes — conditions that frequently accompany MASLD.[5]
A well-planned plant-based diet is another effective option, particularly for those who prefer to minimize animal products. The key is ensuring adequate protein — lentils, tempeh, tofu, edamame, and quinoa can all cover this effectively.
One thing worth pushing back on here: these three patterns are often presented as equivalent options. But the Mediterranean diet has substantially stronger evidence specifically for liver fibrosis outcomes. DASH is primarily studied for its cardiovascular and blood pressure benefits. If liver fat reduction is the primary goal, Mediterranean-style eating is the more directly evidence-supported starting point — though combining elements of all three is both practical and effective.
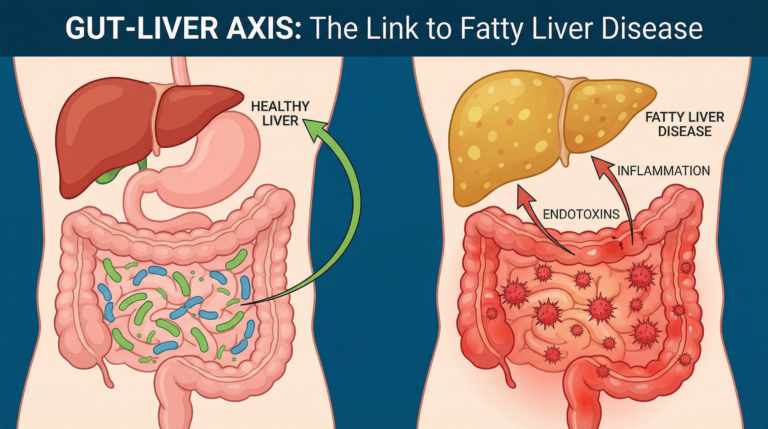
What often gets underestimated in all three approaches is the role the gut microbiome plays in how dietary changes translate into liver outcomes — the gut-liver axis explains why fiber and fermented foods matter beyond their nutritional value alone.
The Role of Supplements and Coffee in Liver Health
This is where the research gets more nuanced — and where standard dietary advice tends to stop too soon.
Omega-3 Fatty Acids and Vitamin E
Omega-3 supplements (fish oil) have been studied in MASLD and show modest but consistent reductions in liver fat and triglycerides when taken alongside dietary changes.[3]
Vitamin E has been studied in non-diabetic adults with biopsy-confirmed steatohepatitis, with some trials showing improvements in liver enzyme levels. However, it is not recommended without medical guidance, particularly at high doses.
One pattern that shows up consistently in the research: supplements perform better as additions to a strong dietary foundation, not as substitutes for one. A fish oil capsule alongside a diet high in refined carbohydrates is unlikely to move the needle much.
Coffee and the Liver
Regular coffee consumption — filtered, without excessive sugar — is associated with reduced liver stiffness and lower fibrosis risk in multiple large studies. One analysis found that drinking two to three cups daily was linked to meaningfully lower markers of liver scarring.[6]
This is one of the more counterintuitive findings in liver research. The benefit appears tied to polyphenols and caffeine’s anti-fibrotic effects, not to any general “detox” mechanism. Skip the sweetened creamers.
Before Starting Any Supplement
Always consult a doctor or registered dietitian before adding supplements — especially if managing type 2 diabetes, obesity, or taking medications. The American Liver Foundation provides practical guidance for those navigating supplementation decisions alongside a liver diagnosis.
Practical Meal Planning for the MASLD Diet
Knowing which foods to eat is the easy part. The harder part is building a consistent weekly structure that actually holds up when life gets busy.
Structuring Meals for Metabolic Balance
Three balanced meals — rather than frequent snacking — tends to support better insulin response throughout the day. This matters specifically for liver fat: each meal triggers an insulin spike, and frequent eating keeps insulin elevated longer, which promotes fat storage in the liver.
A simple structure worth trying:
- Breakfast: Eggs with sautéed greens and whole-grain toast, or Greek yogurt with berries and ground flaxseed
- Lunch: Large salad with chickpeas, olive oil dressing, cucumber, and a boiled egg or grilled chicken
- Dinner: Baked salmon or lentil stew with roasted broccoli and a small portion of brown rice or quinoa
Meal Prep Habits That Make It Sustainable
Batch-cooking legumes (lentils, chickpeas) at the start of the week removes one of the biggest barriers: not having the right food available when hungry.
Keeping a jar of olive oil on the counter and a bag of frozen leafy greens in the freezer are small defaults that quietly shift the diet in the right direction. Progress with managing fatty liver disease tends to come from accumulated daily habits — not from dramatic overhauls.
| Strategy | Liver Benefit | Simple Action |
|---|---|---|
| Three Meals Daily | Reduces insulin exposure and supports metabolic balance | Set consistent times; avoid grazing between meals |
| Weekly Prep | Reduces reliance on processed convenience foods | Cook a large batch of legumes or grains on Sunday |
| Half-Plate Vegetables | Increases fiber; supports blood sugar control | Build every plate around vegetables first, then add protein |
| Limit Added Sugar | Reduces hepatic de novo lipogenesis | Swap sweetened drinks for water, plain coffee, or unsweetened tea |
Lifestyle Factors That Work Alongside Diet
Diet is the most direct lever for liver fat reduction, but it doesn’t work in isolation. Two other factors have strong independent evidence: movement and sleep.
Physical Activity
Losing 5–10% of body weight through a combination of dietary change and regular movement is consistently associated with measurable reductions in liver fat. Current guidance suggests roughly 150 minutes of moderate activity per week — about 20–25 minutes most days.
Both aerobic exercise (brisk walking, cycling) and resistance training show benefit. Resistance training in particular may improve insulin sensitivity independently of weight loss — which matters for the underlying metabolic driver of MASLD.[4]
Short walks after meals are worth noting separately. Research suggests that even a 10-minute walk after eating may help reduce post-meal glucose spikes — one of the key metabolic stressors on the liver.
Sleep and Stress
Chronic sleep restriction elevates cortisol and disrupts insulin sensitivity — both of which promote liver fat accumulation. This is rarely discussed in standard dietary advice for MASLD, but the metabolic data is clear.
Prioritizing 7–9 hours of sleep is not peripheral lifestyle advice. Hormonal shifts also interact with liver metabolism in ways that are easy to overlook — fatty liver and estrogen balance covers how this connection plays out, particularly during perimenopause when liver fat risk rises alongside hormonal change.

Conclusion
The MASLD diet isn’t about eating perfectly — it’s about building a consistent pattern that gives your liver what it needs to do its job.
Prioritizing vegetables, whole grains, lean protein, and healthy fats while limiting added sugars and ultra-processed foods is a well-supported, practical approach. Paired with regular movement and adequate sleep, these changes can produce meaningful improvements in liver fat and metabolic markers.
Small, consistent shifts — a handful more vegetables, an extra serving of fish, less sweetened food — add up over weeks and months. The research supports this approach, and so does the experience of many people who have made these changes and felt the difference. You can do this.
Frequently Asked Questions
What is the MASLD diet and does it really help?
The MASLD diet is a dietary approach centered on whole, anti-inflammatory foods that reduce liver fat and support metabolic health. It emphasizes vegetables, fiber-rich foods, healthy fats like olive oil, lean protein, and limited added sugars. Research suggests that consistently following the MASLD diet — particularly a Mediterranean-style pattern — may reduce liver fat, lower inflammation markers, and slow or prevent the progression of liver damage. Results vary by individual, but dietary changes are considered the primary first-line intervention for most people with this condition.
Is the Mediterranean diet the best choice for MASLD?
Among structured eating patterns, the Mediterranean diet has the strongest evidence specifically for reducing liver fibrosis risk in people with MASLD. A study of over 3,000 adults found that high adherence was associated with a 32% lower risk of advanced liver scarring. DASH and plant-based patterns also show benefit — particularly for people who also have high blood pressure or prefer minimal animal products — but the Mediterranean approach is the most directly studied for liver outcomes.
How much weight do I need to lose to see improvement in liver health?
Research consistently shows that losing 5–10% of body weight — through a combination of dietary changes and regular physical activity — is associated with measurable reductions in liver fat and improvement in liver enzyme levels. For a 180 lb person, that’s roughly 9–18 lbs. Steady, sustainable loss through whole-food dietary changes produces better long-term outcomes than rapid or extreme approaches.
Are there supplements that support liver health in MASLD?
Omega-3 fatty acids and vitamin E are the most studied supplements for MASLD. Omega-3s (from fish oil) may help reduce liver fat and triglycerides when taken alongside a healthy diet. Vitamin E has shown benefit in some trials for people with steatohepatitis, but is not recommended without medical supervision. Coffee — two to three cups daily, without excessive sugar — is also associated with lower liver stiffness markers in multiple large studies. Always consult a doctor before adding supplements, particularly if managing diabetes or taking other medications.
Medical Disclaimer: The information provided in this article is for educational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before making changes to your diet, lifestyle, or treatment plan. TheMetabolicHub.com does not replace professional medical guidance.
References
- Rinella ME et al. MASLD nomenclature and diagnostic criteria. Hepatology. 2023. PMID: 37199328
- Kontogianni MD et al. Mediterranean diet adherence and liver fibrosis risk in MASLD: a study of 3,325 adults. Frontiers in Nutrition. 2023. PMID: 37615200
- Scorletti E, Byrne CD. Omega-3 fatty acids and non-alcoholic fatty liver disease. Molecular Aspects of Medicine. 2018. PMID: 29475058
- European Association for the Study of the Liver (EASL). EASL-EASD-EASO Clinical Practice Guidelines for the Management of Non-Alcoholic Fatty Liver Disease. Journal of Hepatology. 2016. Available at: journal-of-hepatology.eu
- Hekmatdoost A et al. DASH diet and liver fat in NAFLD. Liver International. 2016. PMID: 26010835
- Kennedy OJ et al. Coffee, caffeine and non-alcoholic fatty liver disease. Alimentary Pharmacology & Therapeutics. 2016. PMID: 26818365
- Mayo Clinic. Nonalcoholic fatty liver disease (NAFLD/MASLD). Available at: mayoclinic.org