Signs of Liver Problems in Non Drinkers: 6 Warning Signs to Know

Persistent fatigue that doesn’t lift after a full night’s sleep. A vague heaviness under your right ribs. Digestion that just feels off — bloating, pale stools, or a vanished appetite. These are easy symptoms to brush off as stress or aging. But in some cases, they point to something the liver has been quietly trying to signal for months.
The signs of liver problems in non drinkers are often missed precisely because most people assume liver disease is an alcohol problem. It isn’t. Metabolic stress, diet, insulin resistance, and genetics all play a significant role — and the liver rarely makes noise until it’s already been struggling for a while.
Why Non-Drinkers Get Liver Problems Too
The liver is the body’s primary filter — processing nutrients, clearing toxins, producing bile, and managing blood sugar regulation simultaneously. It’s resilient, but that resilience has a limit.
MASLD (metabolic dysfunction-associated steatotic liver disease — the updated clinical term for what was formerly called NAFLD) is now the most common liver condition globally, and it has nothing to do with alcohol.[1] It develops when fat accumulates in liver cells due to metabolic stress: excess dietary sugar, insulin resistance, central obesity, or some combination of all three.
What makes MASLD particularly tricky is its silence. Fat can build up in the liver for years before any symptoms appear — and by the time symptoms do show up, some degree of inflammation or early fibrosis may already be underway.
This isn’t a personal failure. The liver doesn’t send pain signals early. Millions of people are living with early-stage MASLD right now and have no idea — because the body simply hasn’t raised the alarm yet. You’re not alone in being caught off guard.

The 6 Signs of Liver Problems in Non Drinkers
None of the following signs are specific to liver disease alone — most can have other explanations. But when several appear together, or when one persists without a clear cause, they’re worth investigating.
1. Persistent, Unexplained Fatigue
Not the kind of tired that a good night’s sleep fixes. This is a heavier, more constant exhaustion — often present even after rest — that can make daily tasks feel disproportionately draining.
When the liver is under metabolic stress, toxins that would normally be cleared can begin to accumulate. Research suggests this contributes to systemic fatigue that doesn’t track with activity levels or sleep quality.
2. Jaundice (Yellowing of Skin or Eyes)
Jaundice is the visible yellowing of the skin and the whites of the eyes. It occurs when bilirubin — a pigment produced when red blood cells break down — isn’t being properly processed.[3]
A healthy liver metabolizes bilirubin efficiently. When liver function is impaired, bilirubin accumulates in the bloodstream and becomes visible in the tissues. This is one of the more recognizable signs, but it typically indicates significant dysfunction — not an early stage.
3. Digestive Changes: Gas, Pale Stool, Appetite Loss
The liver produces bile, which is essential for fat digestion and gives stool its characteristic brown color. When bile production or flow is disrupted, digestion becomes inefficient.
Common digestive signs to note:
- Persistent bloating or gas, particularly after fatty meals
- Pale, clay-colored, or greasy stools
- A sudden drop in appetite or persistent nausea
- A feeling of fullness after small amounts of food
Individually, these are common complaints. Together — especially when sustained — they can point to impaired liver function.
4. Abdominal Discomfort (Upper Right Side)
The liver sits under the right ribcage. When it becomes inflamed or enlarged, the surrounding capsule stretches — which can produce a dull ache, pressure, or tenderness in the upper right abdomen.
This discomfort is often mild and easy to dismiss as a pulled muscle or digestive issue. But if it’s consistent, specifically located under the right ribs, and not related to exertion or food, it’s worth mentioning to a doctor.
5. Easy Bruising or Slow Wound Healing
The liver produces clotting factors — proteins that allow blood to clot properly after an injury. When liver function is compromised, clotting factor production drops.
The result: bruises from minor bumps, cuts that take longer than expected to stop bleeding, or a general sense that the body isn’t healing as efficiently as it used to. This sign is more associated with moderate-to-significant liver impairment than with early-stage disease.
6. Unexplained Weight Loss
Losing weight without changing diet or activity level sounds appealing — but unintentional weight loss is a red flag across many conditions, liver disease included.
When the liver is under significant stress, it can impair the body’s ability to process nutrients properly. Appetite often drops. Muscle mass may decrease. The weight loss that follows isn’t a metabolic improvement — it’s the body struggling to maintain normal function.
| Sign | What It May Indicate | Typical Stage |
|---|---|---|
| Persistent Fatigue | Toxin accumulation, metabolic strain | Early to moderate |
| Jaundice | Impaired bilirubin processing | Moderate to advanced |
| Digestive changes | Reduced bile production or flow | Early to moderate |
| Upper right abdominal pain | Liver inflammation or enlargement | Moderate |
| Easy bruising | Reduced clotting factor production | Moderate to advanced |
| Unexplained weight loss | Impaired nutrient processing | Moderate to advanced |
When to See a Doctor
- Vomiting blood or material that looks like coffee grounds
- Sudden, severe abdominal pain
- Rapid onset of jaundice
- Confusion, extreme disorientation, or difficulty staying awake
Schedule a routine appointment if:
- Two or more of the 6 signs above are present for more than 2–3 weeks
- You have known risk factors: insulin resistance, prediabetes, metabolic syndrome, elevated triglycerides, or a family history of liver disease
- Your last liver enzyme panel was abnormal, or you’ve never had one
What You Can Actually Do
One thing worth pushing back on here: the standard advice for liver health tends to stop at “eat less sugar and lose some weight.” That’s not wrong — but it undersells the real driver. For most people with early MASLD, the root issue is insulin resistance, not just caloric excess. Addressing insulin sensitivity directly — through meal composition, movement timing, and sleep — tends to produce faster liver improvements than calorie restriction alone.
The research here is more encouraging than most people expect. Meaningful reductions in liver fat content have been observed in some studies within 8–12 weeks of consistent dietary changes — even without significant weight loss.[1]
Practical starting points that have real evidence behind them:
- Reduce refined carbohydrates and added sugars — fructose in particular drives hepatic fat accumulation via de novo lipogenesis. Swap sugary drinks and processed snacks for whole food sources: lentils, oats, eggs, leafy greens, roasted vegetables.
- A 10–15 minute walk after your largest meal reduces postprandial glucose spikes and directly lowers the metabolic load on the liver. It sounds minor; the glucose data suggests otherwise.
- Prioritize sleep — one week of sleep deprivation has been linked to a 30–40% reduction in insulin sensitivity in research settings. Poor sleep is a direct metabolic stressor for the liver, yet it rarely features in standard liver health guidance.
- Aim for 150 minutes of moderate movement weekly — roughly 20–25 minutes daily. Resistance training 2–3 times per week has additional benefit for insulin-mediated glucose uptake.
What tends to change first when these habits take hold: energy levels in the afternoon often stabilize within 1–2 weeks. Post-meal crashes become less severe. Fasting glucose may begin to drop within 4–8 weeks. For some people, liver enzyme levels normalize within 12 weeks — though this varies considerably by starting point and consistency.
For people with insulin resistance or those exploring MASLD dietary changes, these same steps form the backbone of a liver-supportive approach.

How Liver Problems Are Diagnosed
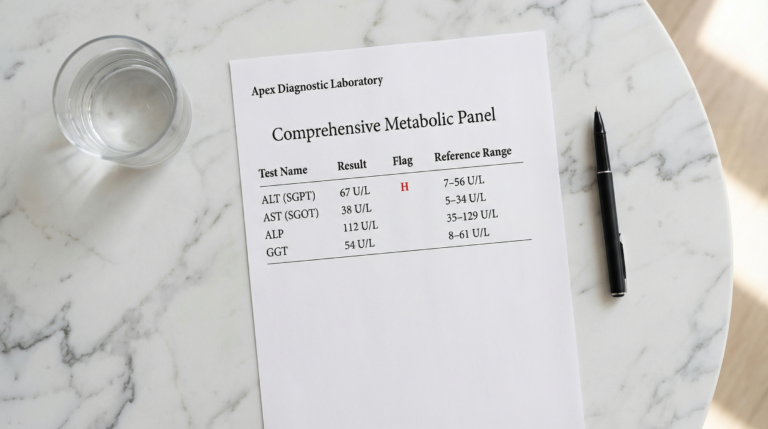
If you’re concerned, the diagnostic process is usually straightforward. It starts with a blood panel.
ALT (alanine aminotransferase) and AST (aspartate aminotransferase) are the two enzymes most commonly used to screen for liver stress.[4] When liver cells are under strain, these enzymes leak into the bloodstream — elevated readings flag the issue. GGT is sometimes included and can be particularly sensitive to metabolic liver stress. A full overview is available in the article on liver enzyme results.
If blood tests come back abnormal, imaging typically follows. Ultrasound is the most common first step — it can detect fat accumulation and changes in liver texture without any radiation. FibroScan (elastography) can assess stiffness, which correlates with fibrosis. MRI is more detailed and used when greater precision is needed.
Biopsy — a small tissue sample taken from the liver — remains the most definitive tool for staging inflammation and fibrosis, though it’s reserved for cases where imaging and blood tests leave diagnostic uncertainty.[5]
Frequently Asked Questions
What are the signs of liver problems in non drinkers?
The most common signs of liver problems in non drinkers include persistent fatigue that doesn’t improve with rest, digestive changes like bloating, pale stools, or appetite loss, and a dull ache or pressure under the right ribs. Jaundice — yellowing of the skin or eyes — is a more visible sign that typically indicates significant dysfunction. Easy bruising and unexplained weight loss can also appear in more advanced cases. These signs are often subtle and overlap with other conditions, which is why many people don’t connect them to the liver until later.
Can you really have liver disease without drinking alcohol?
Yes — and it’s increasingly common. MASLD (metabolic dysfunction-associated steatotic liver disease, formerly NAFLD) is now the most prevalent liver condition globally and has no connection to alcohol consumption. It develops in response to metabolic factors: insulin resistance, excess dietary sugar, central obesity, and genetics. Other non-alcohol causes include certain medications, autoimmune conditions, and viral hepatitis.
How is MASLD different from alcohol-related liver disease?
The underlying trigger differs, but the progression can look similar. Alcohol-related liver disease is caused by the toxic effects of alcohol metabolism on liver cells. MASLD is driven by metabolic dysfunction — excess fat accumulation in liver cells due to insulin resistance and dietary factors. Both can progress through inflammation, fibrosis, and cirrhosis if unmanaged. A fuller comparison is available in the article on alcoholic vs non-alcoholic fatty liver disease.
What blood tests check for liver problems?
A standard liver function panel measures ALT, AST, ALP, and GGT — enzymes that rise when liver cells are under stress — alongside bilirubin and proteins like albumin that reflect the liver’s synthetic function. ALT is considered the most specific marker for hepatocellular injury. These tests are typically included in routine bloodwork, but if you have risk factors for MASLD, it’s worth requesting them specifically and tracking trends over time.
Can lifestyle changes actually improve liver health?
For early-stage MASLD — simple steatosis and early inflammation — research suggests that consistent lifestyle changes can lead to meaningful improvement in liver fat content and enzyme levels, sometimes within 8–12 weeks. The liver has a notable capacity for regeneration when the metabolic stress driving the damage is reduced. More advanced fibrosis is harder to address, which is why early intervention matters. The key levers are dietary changes that support insulin sensitivity, regular physical activity, and sleep quality.
Medical Disclaimer: The information provided in this article is for educational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before making changes to your diet, lifestyle, or treatment plan. TheMetabolicHub.com does not replace professional medical guidance.
References
- Rinella ME et al. A multisociety Delphi consensus statement on new fatty liver disease nomenclature. Hepatology. 2023. PMID: 35066504
- Fevery J. Bilirubin in clinical practice: a review. Liver Int. 2008. PMID: 33065930
- Newsome PN et al. Guidelines on the management of abnormal liver blood tests. Gut. 2018. PMID: 34555398
- European Association for the Study of the Liver. EASL Clinical Practice Guidelines. J Hepatol. 2018. PMC: PMC3933762
- American Liver Foundation. Non-Alcoholic Fatty Liver Disease (NAFLD/MASLD). liverfoundation.org
- Mayo Clinic. Nonalcoholic fatty liver disease — Symptoms & causes. mayoclinic.org