7 Early Warning Signs of a Sluggish Liver You Shouldn’t Ignore

The tiredness hits every afternoon without fail. Sleep doesn’t fix it. Neither does coffee. And no matter how carefully food choices are made, the scale barely moves.
These patterns are easy to blame on stress, age, or willpower. But when several show up together — fatigue, digestive changes, abdominal weight gain, brain fog, or unusual stool changes — they may point to a broader metabolic pattern worth taking seriously.
This guide walks through seven sluggish liver symptoms that may overlap with liver stress, bile-flow issues, fatty liver risk, or metabolic dysfunction — and shows you how to tell the difference between vague symptoms, meaningful patterns, and red flags that deserve medical attention.
Quick Win
Start with one low-risk lever: replace one ultra-processed meal or snack per day with a whole-food option built around protein, fiber, and colorful vegetables. Add cruciferous or bitter greens when possible — broccoli, arugula, kale, Brussels sprouts, or endive. This supports metabolic health and normal liver function without relying on detox products or supplements.
What “Sluggish Liver” Actually Means
“Sluggish liver” is not a medical diagnosis. It is a popular wellness and search term — and in this article, it is used carefully to describe symptom patterns that may overlap with liver stress, impaired bile flow, early MASLD (metabolic dysfunction-associated steatotic liver disease), or broader metabolic dysfunction.
This distinction matters. Most early liver problems — including early-stage fatty liver disease — cause no clear symptoms at all.[1] That means the signs below should never be used for self-diagnosis. They are patterns worth tracking, especially when several appear together, not proof of liver disease.
Standard liver enzyme tests — ALT, AST, GGT — are useful, but incomplete. They can remain normal even when fatty liver or fibrosis risk is present, especially in people with insulin resistance, type 2 diabetes, abdominal weight gain, or high triglycerides.[2] Understanding what liver enzyme results actually mean helps explain what standard panels can and cannot detect.
What Can Put Pressure on the Liver?
The most common contributors include excess dietary fructose, sugary drinks, and ultra-processed foods, which can increase hepatic fat accumulation through de novo lipogenesis — the process by which the liver converts excess carbohydrate into fat.[3]
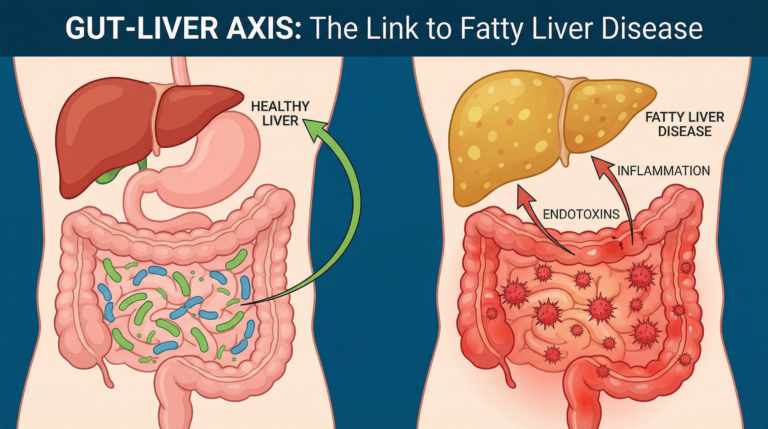
Alcohol, visceral fat, insulin resistance, poor sleep, and chronic inflammation can also increase the liver’s metabolic workload. Gut health matters too: because much of the blood reaching the liver comes from the intestines through the portal vein, the gut and liver are closely connected.[4]
7 Early Signs That May Overlap With Liver Stress
Sign #1: Persistent Fatigue That Sleep Doesn’t Fix

Fatigue is one of the most commonly searched sluggish liver symptoms — and also one of the least specific. Thyroid dysfunction, anemia, poor sleep, chronic stress, depression, low calorie intake, and blood sugar swings can all cause persistent tiredness.
That said, fatigue can appear in people with MASLD and broader metabolic dysfunction.[5] When the liver is under metabolic stress, blood glucose regulation, inflammation, and energy metabolism may become less stable. The result can feel like an afternoon crash that sleep alone does not fully explain.
What to watch for: Fatigue that is worse after meals or in the afternoon, especially when it appears with abdominal weight gain, high triglycerides, poor sleep, or blood sugar dips.
Sign #2: Digestive Discomfort After Fatty Meals
The liver produces bile, which is stored in the gallbladder and released into the small intestine to help digest fat. When bile production or bile flow is impaired, fat digestion can become noticeably uncomfortable.
Bloating, nausea, a heavy sensation in the upper right abdomen, or loose stools after high-fat meals — fried food, cream sauces, rich cheeses, fatty meat — may point to bile, gallbladder, or liver-related issues. This pattern deserves medical evaluation if it is persistent or worsening.
Bile acids also help regulate gut motility and interact with the microbiome. When bile flow is disrupted, digestion and microbial balance can shift, creating a feedback loop between the gut and liver. The gut-liver axis and fatty liver disease covers this connection in more depth.
What to watch for: Symptoms that reliably appear after fatty meals, especially if they occur with pale, greasy, or difficult-to-flush stools.
Sign #3: Itching, Yellowing, or Skin Changes
Some skin changes are clinically important and should not be brushed off. Two signs matter most:
- Generalized itching without a visible rash can occur when bile flow is impaired and bile-related compounds accumulate in the bloodstream.
- Yellowing of the skin or whites of the eyes — jaundice — reflects elevated bilirubin and requires prompt medical attention.
Other skin concerns are less specific. Dullness, breakouts, and hormonal acne can involve stress, sleep, skincare, diet, gut health, insulin resistance, or hormone shifts. They are worth noting if they appear alongside fatigue, abdominal weight gain, high triglycerides, or digestive symptoms, but they are not reliable liver symptoms on their own. The relationship between liver health and estrogen metabolism explains where these patterns may intersect.
What to watch for: Itching without a rash, or any yellowing of the eyes or skin. These signs deserve medical evaluation.
Sign #4: Weight Loss Feels Harder Than Expected
Fatty liver, insulin resistance, elevated insulin, poor sleep, and visceral fat can all make weight loss feel harder by affecting hunger, energy, glucose regulation, and fat metabolism. Calorie balance still matters, but the metabolic environment can make that balance harder to achieve and maintain.
When insulin is chronically elevated — a pattern often seen alongside fatty liver and metabolic syndrome — the body may become less efficient at switching between stored and incoming fuel.[6] That does not make weight loss impossible, but it does mean that “just eat less” often misses the larger mechanism.
Researchers now consider fatty liver disease and metabolic syndrome to be closely overlapping expressions of metabolic dysfunction, not completely separate conditions.
What to watch for: Stalled weight loss despite consistent effort, especially when combined with abdominal fat, high fasting triglycerides, low HDL, elevated glucose, or insulin resistance.
Sign #5: Brain Fog and Low Mental Clarity

In advanced liver disease, impaired ammonia clearance can contribute directly to cognitive symptoms. In earlier metabolic dysfunction, brain fog is more often linked to blood sugar variability, poor sleep, inflammation, insulin resistance, stress, or under-eating.
That distinction is important. Brain fog is not a specific early liver symptom. But when it appears together with fatigue, weight resistance, digestive changes, and abnormal metabolic markers, it may point to a broader metabolic pattern worth evaluating.
What to watch for: Mental sluggishness that worsens after meals, in the afternoon, after poor sleep, or during high-stress periods — especially if other signs on this list also apply.
Sign #6: Stool Color or Bowel Habit Changes
Bile gives stool its characteristic brown color. Pale, clay-colored, or persistently greasy stools can indicate that bile is not reaching the intestine in adequate amounts. This is a meaningful flag for bile flow problems and should be discussed with a healthcare professional.
Very dark or tar-like stools, or any blood in the stool, require prompt medical attention because they may indicate gastrointestinal bleeding. Persistent constipation can also occur when bile acids are low, since bile acids help stimulate intestinal motility, though constipation alone has many possible causes.
What to watch for: Pale, clay-colored, greasy, black, tar-like, or bloody stools. These are not symptoms to self-treat.
Sign #7: Hormonal Symptoms Alongside Metabolic Signs
The liver participates in steroid hormone metabolism, including estrogen, testosterone, cortisol, and DHEA. But hormonal symptoms rarely come from the liver alone.
PMS severity, cycle irregularity, hormonal acne, low libido, mood instability, and perimenopausal symptoms can involve multiple systems: ovaries, thyroid function, stress hormones, sleep, body fat, insulin resistance, inflammation, and medication use.
The liver becomes more relevant when hormonal symptoms appear alongside metabolic signs such as abdominal weight gain, high triglycerides, insulin resistance, fatigue, or fatty liver risk. In that context, it may be more useful to evaluate the broader metabolic picture rather than treating each symptom in isolation.[7]
What to watch for: Hormonal symptoms that persist despite standard management and appear together with fatigue, weight resistance, high triglycerides, or blood sugar problems.
What Can Actually Support Liver Health
The research on early metabolic liver stress is encouraging. Hepatic fat and fasting metabolic markers can improve with consistent nutrition, movement, sleep, and alcohol reduction — especially when changes target insulin resistance and excess liver fat rather than short-term “detox” ideas.
The highest-leverage starting points:
- Reduce ultra-processed foods and sugary drinks. Fructose-heavy diets can accelerate hepatic fat accumulation, especially when overall metabolic risk is already present.
- Reduce or avoid alcohol if fatty liver, high triglycerides, insulin resistance, or abdominal weight gain are present. Alcohol adds metabolic load to the liver and can worsen liver injury risk in vulnerable people.
- Prioritize protein, fiber, legumes, and whole vegetables. Cruciferous vegetables — broccoli, Brussels sprouts, kale — and bitter greens like arugula and endive provide compounds involved in normal liver metabolism and bile production. They are supportive, not curative.
- Improve sleep quality. Poor sleep worsens insulin sensitivity, appetite regulation, cortisol rhythm, and glucose control — all of which affect liver health.
- Add regular physical activity. Even moderate exercise, including walking, improves insulin sensitivity and can reduce liver fat independent of major weight loss.
- Consider appropriate testing if several signs apply: liver panel, fasting glucose or A1c, fasting lipids including triglycerides, and possibly a liver ultrasound depending on risk profile.
For a structured food-based starting point, the best foods for liver health covers evidence-based options in more detail.
| Common Mistake | Why It Backfires | Better Approach |
|---|---|---|
| Jumping to “liver detox” products | Some high-dose herbs or supplements can stress the liver; none replace nutrition, alcohol reduction, sleep, or movement | Use whole-food support: protein, fiber, vegetables, legumes, and reduced added sugar |
| Treating each symptom separately | Fatigue, weight resistance, and hormone symptoms may share metabolic drivers | Look at the metabolic pattern: triglycerides, glucose, insulin resistance, waist circumference, and liver risk |
| Relying only on enzyme tests | ALT, AST, and GGT can be normal even when fatty liver or fibrosis risk is present | Discuss fasting lipids, glucose/A1c, insulin resistance markers, and whether ultrasound is appropriate |
When to See a Doctor
Many symptoms associated with metabolic stress are functional and can improve with lifestyle changes. But some signs require prompt medical evaluation:
- Yellowing of the skin or whites of the eyes
- Dark urine that looks tea-colored or orange-brown
- Pale, clay-colored, black, tar-like, or bloody stools
- Severe or persistent upper right abdominal pain
- Persistent vomiting
- Swelling in the abdomen or legs
- Confusion, disorientation, or unusual sleepiness
- Unexplained weight loss
- Symptoms lasting more than four weeks or getting worse
If several signs apply but standard labs look “normal,” ask whether a broader metabolic and liver evaluation makes sense. Depending on your risk profile, this may include fasting triglycerides, HDL, glucose or A1c, insulin resistance markers, liver enzymes, and imaging such as ultrasound.
Frequently Asked Questions
Can sluggish liver symptoms appear even if my liver enzymes are normal?
Yes. ALT, AST, and GGT are useful markers, but normal liver enzymes do not always rule out fatty liver or fibrosis risk. This is especially important in people with insulin resistance, type 2 diabetes, high triglycerides, abdominal weight gain, or other metabolic risk factors. A healthcare provider may consider additional markers or imaging depending on the full clinical picture.
How quickly can liver health improve with lifestyle changes?
Research on MASLD and fatty liver disease suggests that liver fat and metabolic markers can improve within weeks to months when changes are consistent. The strongest levers are reducing ultra-processed foods, added sugar, excess fructose, and alcohol while improving physical activity, sleep, and insulin sensitivity. Symptoms alone are not the best way to track progress; appropriate labs and imaging are more reliable.
What foods genuinely support liver health?
The most evidence-aligned approach is a whole-food dietary pattern: adequate protein, legumes, vegetables, fiber-rich carbohydrates, olive oil, nuts, fish, and minimal ultra-processed foods or sugary drinks. Cruciferous vegetables and bitter greens can support normal liver metabolism and bile production, but no single food detoxes the liver on its own.
Is a sluggish liver the same as fatty liver disease?
No. “Sluggish liver” is not a medical diagnosis. Fatty liver disease, now often referred to as MASLD when linked to metabolic dysfunction, is diagnosed through clinical evaluation, imaging, and sometimes additional testing. The term “sluggish liver” can describe symptom clusters that overlap with liver or metabolic stress, but it should not be treated as a diagnosis.
Can stress contribute to sluggish liver symptoms?
Stress is unlikely to cause liver disease by itself, but chronic stress can worsen the metabolic environment that affects liver health. Elevated cortisol, poor sleep, higher blood glucose, emotional eating, and reduced activity can all increase insulin resistance and visceral fat over time. This is why liver health is best approached through the whole metabolic pattern, not one isolated habit.
Conclusion
Sluggish liver symptoms rarely tell a simple story. Fatigue, brain fog, weight resistance, digestive discomfort, stool changes, or hormone symptoms can each have many explanations. But when several overlap — especially alongside abdominal weight gain, high triglycerides, insulin resistance, or fatty liver risk — they may point to a metabolic pattern worth evaluating.
The strongest starting points are not detox teas or complicated supplement protocols. They are the basics that consistently move liver and metabolic health: fewer ultra-processed foods, less added sugar and alcohol, more protein and fiber, regular movement, better sleep, and appropriate testing when symptoms persist.
When improvement happens, it often shows up first in energy, digestion, or metabolic markers — but the safest way to track liver health is with proper evaluation, not symptoms alone.
Medical Disclaimer: The information provided in this article is for educational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before making changes to your diet, lifestyle, supplements, medications, or treatment plan. TheMetabolicHub.com does not replace professional medical guidance.
References
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). NAFLD & NASH. niddk.nih.gov
- Rinella ME, Neuschwander-Tetri BA, Siddiqui MS, et al. AASLD Practice Guidance on the clinical assessment and management of nonalcoholic fatty liver disease. Hepatology. 2023;77(5):1797–1835. PMID: 36727674
- Softic S, Cohen DE, Kahn CR. Role of dietary fructose and hepatic de novo lipogenesis in fatty liver disease. Dig Dis Sci. 2016;61(5):1282–1293. PMID: 26856717
- Tripathi A, Debelius J, Brenner DA, et al. The gut-liver axis and the intersection with the microbiome. Nat Rev Gastroenterol Hepatol. 2018;15(7):397–411. PMID: 29748586
- Mayo Clinic. Metabolic dysfunction-associated steatotic liver disease (MASLD) — Symptoms and causes. mayoclinic.org
- Marchesini G, Brizi M, Bianchi G, et al. Nonalcoholic fatty liver disease: a feature of the metabolic syndrome. Diabetes. 2001;50(8):1844–1850. PMID: 11473047
- Targher G, Corey KE, Byrne CD, Roden M. The complex link between NAFLD and type 2 diabetes mellitus — mechanisms and treatments. Nat Rev Gastroenterol Hepatol. 2021;18(9):599–612. PMID: 33972770