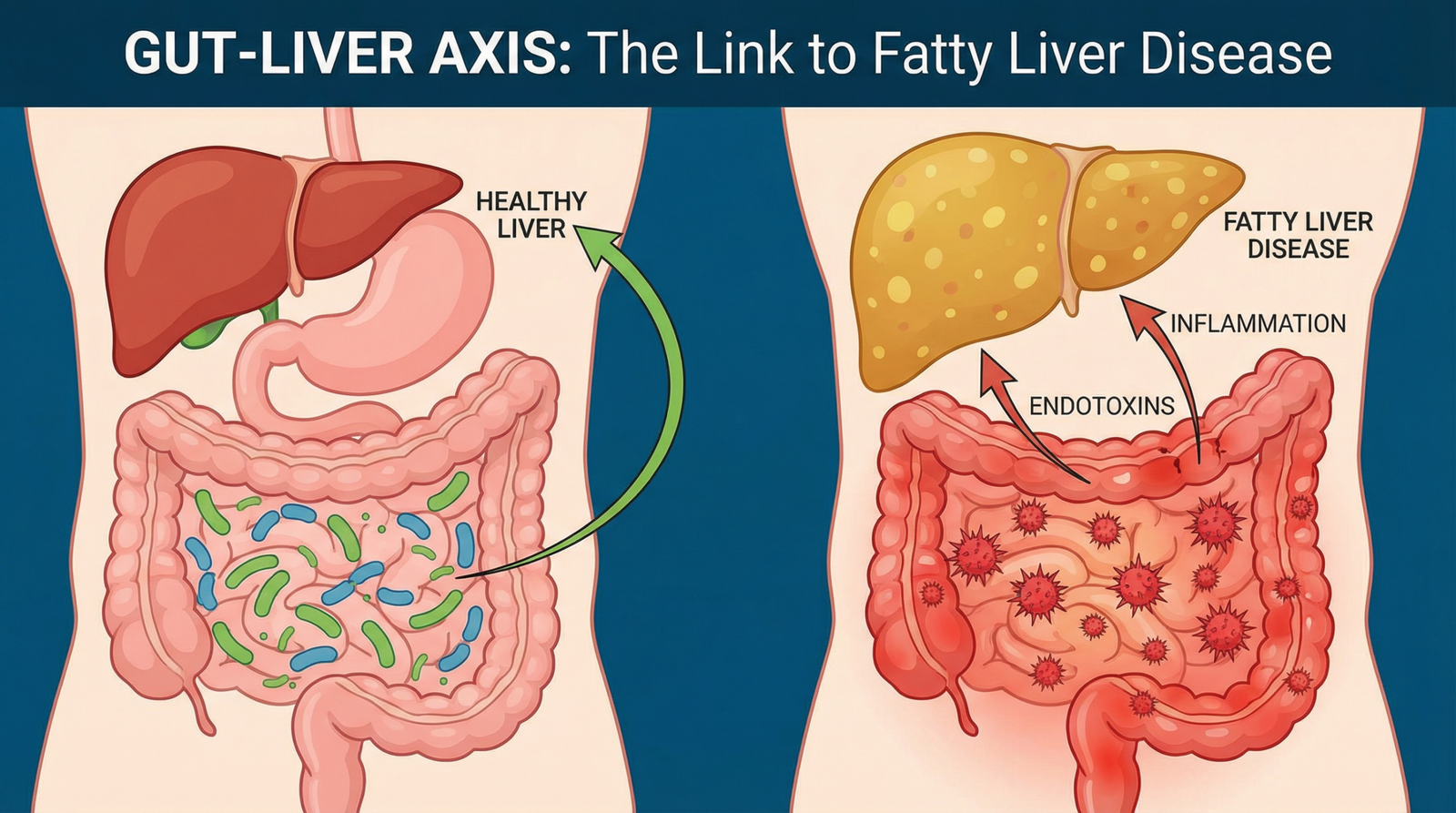
The Gut-Liver Axis and Fatty Liver: Why Your Digestive Health Matters
You may have been told your liver needs attention — elevated enzymes, a fatty liver finding on an ultrasound, or a doctor’s note about NAFLD. What often doesn’t get explained is why it happened.
For many adults, the answer isn’t just diet or alcohol. It starts much further up the digestive tract. The gut-liver axis and fatty liver disease are more tightly connected than most people realize — and that connection is where both the problem and the solution often begin.
The encouraging news: the gut-liver axis fatty liver relationship is one of the most actionable areas in metabolic health research right now. Changes in diet and lifestyle can measurably shift how this system functions — often within weeks.
| Key Takeaway | What It Means for You |
|---|---|
| Gut and liver talk constantly | Via the portal vein, bile acids, and microbial metabolites — disruption in one affects the other directly |
| Dysbiosis drives fat accumulation | An imbalanced gut microbiome sends inflammatory signals that promote liver fat storage |
| Leaky gut is a key mechanism | When the intestinal barrier weakens, bacterial toxins travel to the liver and trigger inflammation |
| Diet is the most powerful lever | Fiber diversity, reduced fructose, and fermented foods directly reshape both gut and liver health |
What Is the Gut-Liver Axis and Why Does It Matter for Fatty Liver?
The gut-liver axis fatty liver connection describes the continuous two-way communication between your intestines and your liver — and how disruption in that communication contributes to fat accumulation in liver tissue.
The main physical route is the portal vein, which carries blood — along with nutrients, bacterial byproducts, and metabolic signals — directly from the intestines to the liver. Everything your gut processes reaches your liver first. When gut balance is disrupted, the liver absorbs the consequences.[1]
Three channels carry these signals back and forth: the portal vein (blood flow), the biliary tract (bile acids cycling between liver and gut), and systemic circulation (immune signals and metabolites). When all three work well, the liver processes fats efficiently and inflammation stays low. When they don’t, fatty liver disease is one of the results.
How Gut Bacteria Influence Liver Fat
Your gut microbiome — the trillions of microbes living in your intestines — directly shapes what your liver has to deal with every day.
Beneficial bacteria ferment dietary fiber and produce short-chain fatty acids like butyrate. Butyrate strengthens the intestinal lining, reduces inflammation, and supports healthy liver metabolism. Harmful bacteria, when they overgrow, produce lipopolysaccharides (LPS) — bacterial toxins that travel through the portal vein and trigger inflammatory responses in the liver.[2]
Research has found that people with nonalcoholic fatty liver disease (NAFLD) consistently show altered microbiome composition — less diversity, lower levels of protective bacteria, and higher levels of bacteria that produce alcohol-like compounds. One study found elevated ethanol production by gut microbiota in pediatric NASH patients — internal alcohol that the liver then had to process, accelerating fat accumulation.[3]
| Microbial Byproduct | Source | Effect on Liver |
|---|---|---|
| Butyrate (SCFA) | Fiber fermentation by beneficial bacteria | Protective — reduces inflammation, supports cell integrity |
| LPS (Endotoxin) | Gram-negative bacteria overgrowth | Harmful — triggers inflammation and fat accumulation |
| Secondary Bile Acids | Bacterial modification of primary bile acids | Mixed — aid metabolism or cause damage in excess |
| Microbial Ethanol | Certain bacteria in dysbiotic gut | Harmful — accelerates hepatic fat storage (steatosis) |
Leaky Gut: The Mechanism That Connects Gut Imbalance to Liver Damage
The intestinal lining is a single layer of cells held together by tight junctions — specialized protein seals that control what passes into the bloodstream.
When tight junctions loosen — from a poor diet, chronic stress, alcohol, or antibiotic overuse — the gut becomes more permeable. Bacterial toxins, undigested food particles, and inflammatory compounds slip through into the portal bloodstream and travel directly to the liver. This is often called “leaky gut,” and research confirms it plays a central role in NAFLD progression.[4]
The liver responds to this constant stream of toxins with inflammation. Over time, chronic low-grade inflammation is what drives the progression from simple fat accumulation (steatosis) to the more serious nonalcoholic steatohepatitis (NASH) — where inflammation and liver cell damage occur together.
The Role of Diet in the Gut-Liver Axis Fatty Liver Connection
Diet is the most direct way to shift the gut-liver axis fatty liver relationship — in either direction.
High-fructose intake is particularly damaging. Fructose is metabolized almost exclusively in the liver, where excess amounts are converted to fat through a process called de novo lipogenesis. At the same time, high-fructose diets alter gut microbiome composition, increasing intestinal permeability and the flow of bacterial toxins to the liver — a double hit.[5]
High-fat processed diets have a similar effect. Research found that a high-fat diet significantly increases gut-derived endotoxemia — the presence of bacterial toxins in the bloodstream — which directly promotes hepatic inflammation.
On the other side: fiber diversity is one of the most protective dietary factors available. A wide variety of plant foods — vegetables like broccoli, artichokes, and leafy greens; legumes like lentils and chickpeas; whole grains like oats and barley — feeds the beneficial bacteria that produce butyrate and maintain gut barrier integrity.
| Dietary Pattern | Effect on Gut Microbiome | Effect on Liver |
|---|---|---|
| High fructose / sugary drinks | Reduces microbial diversity, increases permeability | Promotes fat accumulation via de novo lipogenesis |
| High processed fat | Increases endotoxin-producing bacteria | Triggers inflammation, worsens insulin resistance |
| High fiber / diverse plants | Increases butyrate-producing bacteria | Reduces inflammation, supports fat metabolism |
| Mediterranean pattern | Increases microbial diversity and resilience | Associated with reduced NAFLD severity |
What You Can Do: Practical Steps to Support the Gut-Liver Axis
The research on the gut-liver axis fatty liver connection points consistently toward the same practical interventions. None of them require a prescription.
Increase fiber variety, not just quantity. Aim for 30 or more different plant foods per week — not 30 servings of the same thing. Rotating vegetables, legumes, fruits, nuts, and whole grains feeds different bacterial species and builds a more resilient microbiome.
Cut sugar-sweetened beverages first. Fructose from sodas and fruit juices is the most direct dietary driver of liver fat. Replacing them with water, sparkling water, or unsweetened herbal tea is the single highest-leverage dietary swap for liver health.
Add fermented foods regularly. Yogurt (plain, unsweetened), kefir, sauerkraut, kimchi, and miso introduce beneficial bacteria and have been shown to improve microbiome diversity. Even small amounts daily — a few tablespoons of sauerkraut, a serving of yogurt — add up over weeks.
Reduce processed and ultra-processed foods. These disrupt tight junction proteins and feed endotoxin-producing bacteria. Cooking from whole ingredients most of the time makes a measurable difference in gut permeability within weeks.
Consider sleep and stress seriously. Chronic stress elevates cortisol, which increases intestinal permeability and suppresses beneficial gut bacteria. Sleep under seven hours per night has similar effects. Both are direct inputs into gut barrier function — not peripheral lifestyle factors.
Move after meals. A 10-minute walk after eating reduces postprandial blood sugar and supports the muscular contractions that keep gut transit healthy. Research suggests short post-meal movement reduces glucose spikes more effectively than one longer session per day.[6]
Bile Acids: The Overlooked Messenger
Bile acids deserve a specific mention because they are often left out of plain-language explanations of liver health.
Your liver produces bile acids to help digest dietary fat. After use in the small intestine, roughly 95% are reabsorbed and sent back to the liver — a recycling loop called enterohepatic circulation. But gut bacteria modify these bile acids along the way, converting them into secondary forms that act as signaling molecules.
These signals regulate blood sugar, cholesterol metabolism, and energy use throughout the body. When the microbiome is imbalanced, this bile acid signaling becomes dysregulated — contributing to insulin resistance and worsening liver fat accumulation. Supporting the gut microbiome through diet directly improves bile acid signaling as a downstream effect.[1]
Conclusion
The gut-liver axis fatty liver connection explains something that standard medical conversations often miss: fatty liver disease is not just a liver problem. It is a systemic condition shaped by what is happening in the gut — microbial balance, intestinal barrier integrity, and the quality of signals traveling through the portal vein every day.
That framing is actually useful, because it means the intervention points are practical and accessible. What you eat, how diverse your plant intake is, whether you are getting enough sleep, how you manage stress — all of these directly influence the gut environment that shapes liver health.
Small, consistent changes compound over time. The biology supports recovery when the right inputs are in place.
Frequently Asked Questions
What is the gut-liver axis and how does it relate to fatty liver disease?
The gut-liver axis fatty liver connection refers to the continuous two-way communication between the intestines and the liver via the portal vein, bile acids, and immune signals. When gut bacteria are imbalanced or the intestinal barrier is weakened, inflammatory toxins travel directly to the liver through the portal bloodstream, promoting fat accumulation and inflammation. Research consistently shows that people with NAFLD have distinct microbiome profiles compared to those with healthy livers — making gut health a central factor in fatty liver prevention and management.
What is leaky gut and does it really cause liver problems?
Leaky gut — clinically called increased intestinal permeability — occurs when the tight junction proteins between intestinal cells loosen, allowing bacterial toxins and undigested compounds to enter the bloodstream. Research has confirmed that people with NAFLD show measurably higher intestinal permeability than healthy controls. These toxins travel through the portal vein to the liver, triggering chronic low-grade inflammation that drives the progression from simple steatosis to the more serious NASH. Improving gut barrier integrity through diet, sleep, and stress management is considered a meaningful intervention for liver health.
Which foods are most harmful for the gut-liver axis?
Sugar-sweetened beverages and high-fructose foods are among the most damaging — fructose is metabolized almost entirely in the liver, where excess amounts are converted directly to fat. High-fat processed foods promote the overgrowth of endotoxin-producing bacteria and increase gut permeability. Ultra-processed foods more broadly disrupt the tight junction proteins that maintain the intestinal barrier. Reducing these categories — particularly sugary drinks — is consistently identified in research as a high-leverage intervention for both gut microbiome health and liver fat reduction.
What is the difference between NAFLD and NASH?
NAFLD (nonalcoholic fatty liver disease) is the broader term for excess fat accumulation in liver cells not caused by alcohol. It ranges from simple steatosis — fat storage without significant inflammation — to NASH (nonalcoholic steatohepatitis), where fat accumulation is accompanied by liver cell inflammation and damage. NASH carries a meaningfully higher risk of progression to fibrosis (scarring) and cirrhosis. The gut-liver axis is implicated in this progression — chronic gut-derived inflammation is one of the key drivers of the transition from benign fat storage to active liver injury.
Can you improve gut health and liver health at the same time?
Yes — and this is one of the most practical aspects of the gut-liver axis research. Dietary changes that improve microbiome diversity, such as increasing fiber variety and reducing processed foods, simultaneously reduce the inflammatory load reaching the liver. Adding fermented foods supports beneficial bacterial populations. Reducing sugar-sweetened beverages lowers both liver fat production and the fructose-driven disruption of gut bacteria. Because the gut and liver are in constant communication, interventions that support one tend to benefit the other through the same biological pathways.
Medical Disclaimer: The information provided in this article is for educational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before making changes to your diet, lifestyle, or treatment plan. TheMetabolicHub.com does not replace professional medical guidance.
References
- Tilg H, Cani PD, Mayer EA. Gut microbiome and liver diseases. Gut. 2016;65(12):2035–2044. PMID: 27802157
- Schnabl B, Brenner DA. Interactions between the intestinal microbiome and liver diseases. Gastroenterology. 2014;146(6):1513–1524. PMID: 24440671
- Zhu L, et al. Characterization of gut microbiomes in nonalcoholic steatohepatitis (NASH) patients. Hepatology. 2013;57(2):601–609. PMID: 22972073
- Miele L, et al. Increased intestinal permeability and tight junction alterations in nonalcoholic fatty liver disease. Hepatology. 2009;49(6):1877–1887. PMID: 19291785
- Pendyala S, et al. A high-fat diet is associated with endotoxemia that originates from the gut. Gastroenterology. 2012;142(5):1100–1101. PMID: 22326433
- Buffey AJ, et al. The acute effects of interrupting prolonged sitting time with standing and light-intensity walking on biomarkers of cardiometabolic health. Sports Med. 2022;52(8):1765–1787. PMID: 35315000
- American Liver Foundation. Nonalcoholic Fatty Liver Disease. Available at: liverfoundation.org
- Harvard T.H. Chan School of Public Health. The Nutrition Source — Fiber. Available at: hsph.harvard.edu