Can Fatty Liver Be Reversed? What the Research Says

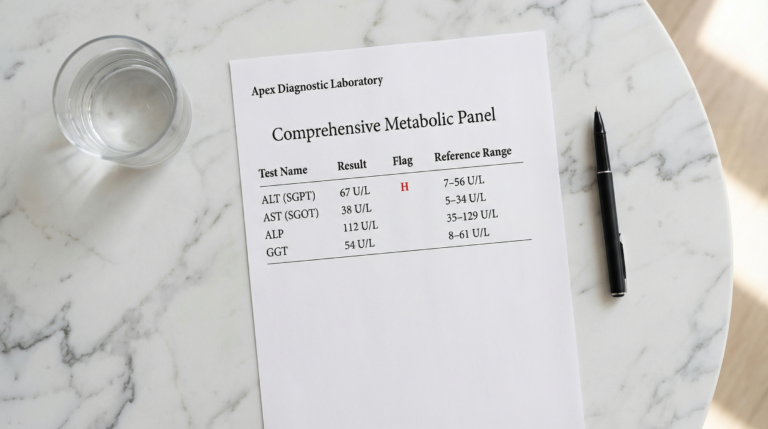
You get a blood test back and the numbers are off. Or an ultrasound flags something unexpected — and suddenly you’re reading about fatty liver disease for the first time, feeling confused and, honestly, a little unsettled.
Here’s what most people aren’t told clearly enough: this is one of the few chronic metabolic conditions where meaningful reversal is genuinely possible — often faster than expected.
Understanding how fatty liver reversed itself in clinical research — and what actually drove those results — is one of the most useful things you can take away from this article. The timeline is faster than most people expect.
Quick Takeaways
- Fatty liver is reversible in early and middle stages — confirmed by liver biopsy and MRI research
- A 7–10% reduction in body weight produces measurable liver improvement in the majority of people with NAFLD
- Liver fat can begin dropping within 2–8 weeks of consistent dietary change
- Exercise reduces liver fat even without weight loss
- Advanced fibrosis (stage 4+) is largely irreversible — which is why early action matters
If you only focus on 3 things:
- Lose 7–10% of your body weight — the most reliably proven threshold for histological improvement
- Reduce sugar and refined carbohydrates — fructose and refined starches are the primary drivers of liver fat synthesis
- Move consistently every day — even a 10–15 minute walk after meals reduces liver fat through mechanisms independent of weight loss
Everything else in this article supports these three. Start here.
In This Article
- What Is Fatty Liver Disease?
- The Real Driver of Liver Fat (Most People Get This Wrong)
- Fatty Liver Reversed: What the Research Shows
- How Fast Does Reversal Happen?
- Diet: What Has the Strongest Evidence
- Exercise: More Powerful Than Most People Realize
- Common Mistakes That Slow Progress
- When Lifestyle Isn’t Enough
- Frequently Asked Questions
What Is Fatty Liver Disease?
Fatty liver disease — clinically called hepatic steatosis — occurs when fat makes up more than 5% of the liver’s total weight.
The liver is not designed to be a fat storage organ. Its job is to filter blood, regulate glucose, produce bile, and process nutrients. When fat accumulates inside liver cells, it disrupts all of these functions — often silently, without symptoms, for years.
Two Main Types
- Alcoholic fatty liver disease (AFLD) — driven by chronic alcohol intake, which forces the liver to prioritize metabolizing ethanol over clearing fat
- Non-alcoholic fatty liver disease (NAFLD / MASLD) — occurs in people who drink little or no alcohol; tightly linked to insulin resistance, visceral fat, and metabolic syndrome
The Stages — and What They Mean for Reversibility
| Stage | What’s Happening | Reversibility |
|---|---|---|
| 1 — Simple Steatosis | Fat accumulates, no significant inflammation yet | Highly reversible |
| 2 — NASH | Fat plus active liver inflammation and cell injury | Highly reversible with intervention |
| 3 — Early Fibrosis | Scar tissue begins forming around liver cells | Meaningful reversal possible |
| 4 — Cirrhosis | Widespread scarring disrupts liver architecture | Largely permanent — progression can be slowed |
| 5 — End-Stage | Liver failure or hepatocellular carcinoma | Requires specialist medical care |
For most people who catch a fatty liver diagnosis before cirrhosis, the window for meaningful reversal is genuinely open.
The Real Driver of Liver Fat (Most People Get This Wrong)
This is where most people — and many generic health articles — get it wrong.
Fatty liver is not primarily caused by eating too much dietary fat. That assumption sounds logical, but the research points somewhere else entirely: insulin resistance and chronic sugar intake are the central drivers.
Here’s the mechanism. When cells stop responding to insulin efficiently — a state called insulin resistance — the pancreas compensates by producing more. Chronically elevated insulin drives the liver to convert excess glucose and fructose into fat through a process called de novo lipogenesis (DNL).
Fructose is particularly problematic. Unlike glucose, fructose is almost entirely metabolized by the liver, flooding it with raw material for fat synthesis. This is why sugar-sweetened drinks, fruit juice, and processed foods high in high-fructose corn syrup are so strongly linked to NAFLD progression — even in people who aren’t overweight.
Refined starches (white bread, white rice, most breakfast cereals) drive the same cascade through a different mechanism: rapid glucose spikes trigger insulin surges, and chronically elevated insulin keeps the liver’s fat-synthesis pathways open.
The practical implication: reducing sugar and refined carbohydrates is more directly impactful for liver fat than reducing dietary fat. Replacing them with fiber-rich whole foods — lentils, chickpeas, farro, oats, non-starchy vegetables — dampens the insulin response and reduces DNL signaling.

Fatty Liver Reversed: What the Research Actually Shows
Yes — and the evidence behind it is substantial.
Studies using liver biopsy and MRI have documented measurable reductions in liver fat — and in some cases complete resolution of liver inflammation (NASH) — in people who sustain dietary and lifestyle changes.
The landmark Vilar-Gomez study followed 293 people with histologically confirmed NASH through a 52-week lifestyle intervention. NASH resolution was observed in those who lost at least 3% of body weight — and among those who lost ≥10%, NASH resolution occurred in 90% of cases.[1]
These are biopsy-confirmed results — not self-reported improvements or surrogate markers.
The pattern of fatty liver reversed through lifestyle change — without surgery or medication — is now one of the most replicated findings in hepatology research.
What About Fibrosis?
Fibrosis — scar tissue in the liver — was previously thought to be one-directional. The research now tells a different story.
In the same cohort, fibrosis regression was observed in 45% of those who achieved ≥10% weight loss. Even those who lost 5–10% showed meaningful fibrosis improvement in a substantial proportion of cases.[1]
The liver has more regenerative capacity than most people — and many doctors — give it credit for.
How Fast Does Reversal Happen?
Faster than most people expect — and faster than almost any other chronic condition.
MRI studies show measurable drops in liver fat within 2–8 weeks of significant dietary change. The liver responds more quickly to dietary intervention than muscle, adipose tissue, or cardiovascular markers.
Fibrosis reversal takes longer — typically 6–12 months or more of sustained change.
What Early Improvement Feels Like
Early signs the liver is responding (often within 2–6 weeks):
- Liver enzyme levels (ALT, AST) begin to drop — often within 4–6 weeks
- Energy in the afternoon stabilizes — less post-lunch fatigue
- Post-meal heaviness and bloating tend to lessen
- Blood sugar levels after meals may become more stable
These shifts often appear before any imaging confirms them. For more on what your liver enzyme results actually mean, the ALT, AST, ALP and GGT explainer on this site covers the lab picture in depth.
Diet: What Has the Strongest Evidence
No single diet produces fatty liver reversed overnight. But several patterns have robust, replicated evidence — and they share key features.
Priority 1: Reduce Sugar and Refined Carbohydrates
This is the highest-impact dietary change for liver fat. The targets: sugar-sweetened drinks, fruit juice, white bread, white rice, most packaged breakfast cereals, and anything with added high-fructose corn syrup.
Replace these with slower-digesting carbohydrates: lentils, chickpeas, black beans, steel-cut oats, farro, bulgur, and non-starchy vegetables. These reduce the insulin response and cut off the primary fuel supply for de novo lipogenesis.
Priority 2: The Mediterranean Pattern
The Mediterranean dietary pattern consistently outperforms low-fat diets in NAFLD research — and reduces liver fat even without caloric restriction.[2]
The likely mechanisms: high monounsaturated fat from olive oil, anti-inflammatory polyphenols, low refined carbohydrate load, and omega-3 fatty acids from oily fish that reduce liver triglyceride synthesis directly.
In practice: sardines, mackerel, or trout 2–3 times per week; olive oil as your primary cooking fat; meals built around legumes and non-starchy vegetables; a significant reduction in processed food.
Priority 3: Meaningful Weight Loss
Across trials, losing 7–10% of total body weight is the most reliable predictor of measurable liver improvement. For someone at 180 lbs, that’s 13–18 lbs. For someone at 220 lbs, roughly 15–22 lbs.
The composition of the diet matters somewhat — but reaching this threshold matters more. Higher-protein, lower-glycemic approaches tend to produce better adherence, which is ultimately what drives results.
Secondary: Coffee
Regular coffee consumption is consistently associated with lower rates of liver fibrosis and slower NAFLD progression — one of the most replicated findings in liver health research.[3]
Two or more cups per day appears protective in meta-analyses. It is not a substitute for dietary change — but it’s a genuine secondary benefit that requires no extra effort.

Exercise: More Powerful Than Most People Realize
Here’s what matters most: exercise reduces liver fat through mechanisms that are partly independent of weight loss.
Even without meaningful changes on the scale, aerobic exercise reduces liver fat — confirmed across multiple controlled trials. The mechanism: moderate-intensity activity activates AMPK (AMP-activated protein kinase) in liver tissue, which shifts the metabolic balance toward fat oxidation and away from fat synthesis. It also improves insulin sensitivity in muscle, reducing the glucose load arriving at the liver.
Aerobic Exercise — The Foundation
Moderate-intensity aerobic movement — brisk walking, cycling, swimming — performed roughly 150 minutes per week (about 20–25 minutes daily) reduces liver fat by a clinically meaningful amount in controlled trials, even when diet is held constant.
A practical starting point: a 10–15 minute walk after the largest meal of the day. Research on post-meal movement shows a measurable effect on glucose and liver fat over time — no equipment, gym membership, or schedule restructuring required.
Resistance Training — Underrated
In a well-designed randomized controlled trial, resistance and aerobic training produced equivalent reductions in hepatic fat content in people with NAFLD and type 2 diabetes (−25.9% resistance vs −32.8% aerobic, both statistically significant).[4]
The benefit comes from increased muscle mass, which improves whole-body insulin sensitivity and reduces baseline insulin levels — cutting off the primary signal for hepatic fat synthesis.
Combining both types produces the largest effect. But the practical message is simpler: any consistent movement helps. Consistency beats intensity, especially at the start.
Common Mistakes That Slow Progress
“Liver Detox” Products
No supplement has strong evidence for producing fatty liver reversed. Milk thistle shows some anti-inflammatory effects in small studies, but no large randomized controlled trial has demonstrated meaningful liver fat reduction.
More importantly: some “liver detox” supplements contain compounds that are hepatotoxic. A 2017 review in Hepatology documented liver injury from herbal and dietary supplements as a significant and growing clinical concern.[5] For a liver already under metabolic stress, that’s the opposite of helpful.
Watching Only the Scale
Weight loss matters — but dietary composition matters too, independently. Swapping refined carbohydrates and sugar for protein and healthy fats produces faster liver fat reduction than the same caloric deficit achieved through low-fat, high-carbohydrate eating.
The number on the scale is a useful proxy. It isn’t the whole picture.
Alcohol — Even “Moderate” Amounts
In people with NAFLD, even moderate alcohol consumption accelerates liver fat accumulation and increases fibrosis risk. The liver cannot simultaneously process alcohol and work toward fatty liver reversed.
For anyone actively working on liver recovery, reducing or eliminating alcohol is foundational — not optional.
Assuming It’s Too Late
Many people sit with a fatty liver diagnosis for months or years without acting, assuming the damage is already done. For most — those without advanced fibrosis or cirrhosis — this assumption is wrong.
The research includes people in their 50s, 60s, and 70s who achieved meaningful liver fat reduction. It is not a failure of willpower that got most people here — it’s years of metabolic signals the body sent without being heard clearly.

When Lifestyle Isn’t Enough
For people with NASH and advanced fibrosis (stage 2–3), lifestyle changes remain first-line treatment. But medications are now available for those who need additional support.
In 2024, resmetirom (Rezdiffra) became the first FDA-approved medication specifically for NASH with liver fibrosis. It works by activating thyroid hormone receptors in the liver (THR-β), increasing hepatic fat oxidation. Clinical trials showed meaningful fibrosis improvement in approximately 26% of patients versus placebo after one year.[6]
GLP-1 receptor agonists — including semaglutide — show strong signals for NASH improvement in ongoing trials. These drugs reduce appetite, support weight loss, and appear to have direct anti-inflammatory effects on liver tissue.
Both work best alongside dietary and lifestyle change — not as replacements for it. If you’ve made consistent changes without sufficient improvement, a conversation with a gastroenterologist or hepatologist is worth having.
The Bottom Line
Fatty liver disease is serious — but it’s also one of the most actionable diagnoses in metabolic medicine.
The research on fatty liver reversed through lifestyle change is clear: for most people in early and middle stages, it happens. Liver fat drops measurably within weeks. Enzyme levels follow. And the interventions that produce these results — reducing sugar and refined carbohydrates, moving consistently, losing a meaningful but achievable amount of weight — are the same ones that improve metabolic health across the board.
Start with the three priorities at the top of this article. The biology will follow.
Frequently Asked Questions
Can fatty liver be reversed?
Yes — research consistently shows fatty liver reversed through sustained lifestyle change in early and middle stages. Biopsy-confirmed studies document complete resolution of liver inflammation (NASH) in up to 90% of people who achieve ≥10% weight loss. The primary drivers are reducing sugar and refined carbohydrates, consistent movement, and meaningful weight loss. Advanced cirrhosis involves structural changes that are largely permanent — which is why acting early matters significantly.
How long does it take to reverse fatty liver?
MRI studies show measurable liver fat reduction within 2–8 weeks of significant dietary change — unusually fast for a chronic condition. Early subjective improvements (more stable energy, less post-meal heaviness) often appear within the first 1–2 weeks. Liver enzymes (ALT, AST) frequently begin to normalize within 4–6 weeks of consistent dietary adjustment. Fibrosis reversal takes longer — typically 6–12 months or more of sustained lifestyle change.
Can fatty liver be reversed without losing weight?
Partially, yes. Aerobic exercise reduces liver fat even without weight loss, and reducing dietary fructose and refined carbohydrates can lower liver fat independent of scale changes. However, weight loss — particularly loss of visceral fat — remains the most reliable driver of full reversal. A 7–10% reduction in body weight is the threshold most consistently associated with histological improvement in research.
How do I know if my fatty liver is improving?
The most direct measure is repeat liver imaging — ultrasound or MRI-PDFF (which quantifies liver fat percentage). Blood markers like ALT and AST often improve as liver fat drops, though they’re not perfect proxies. Subjectively, many people notice improved energy, less afternoon fatigue, and reduced post-meal bloating before lab values shift. Your doctor may recommend repeat imaging after 3–6 months of sustained lifestyle change to assess progress objectively.
What is the best diet to support fatty liver reversed?
The Mediterranean dietary pattern has the strongest replicated evidence for NAFLD improvement. Key elements: significantly reducing sugar and refined carbohydrates (sweetened drinks, white bread, packaged cereals), emphasizing oily fish (sardines, mackerel), olive oil, legumes like lentils and chickpeas, and non-starchy vegetables. Regular coffee consumption (2+ cups per day) is associated with lower fibrosis risk in meta-analyses. The MASLD diet guide on this site covers practical meal structure in more detail.
Medical Disclaimer: The information provided in this article is for educational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before making changes to your diet, lifestyle, or treatment plan. TheMetabolicHub.com does not replace professional medical guidance.
References
- Vilar-Gomez E, et al. Weight Loss Through Lifestyle Modification Significantly Reduces Features of Nonalcoholic Steatohepatitis. Gastroenterology. 2015;149(2):367–78.
PMID: 25865049 - Kontogianni MD, et al. Adherence to the Mediterranean diet is associated with lower prevalence of non-alcoholic fatty liver disease. Metabolism. 2014.
PMID: 28371239 - Kennedy OJ, et al. Systematic review with meta-analysis: coffee consumption and the risk of cirrhosis. Aliment Pharmacol Ther. 2016;43(5):562–74.
PMID: 26806124 - Bacchi E, et al. Both resistance training and aerobic training reduce hepatic fat content in type 2 diabetic subjects with NAFLD (the RAED2 Randomized Trial). Hepatology. 2013;58(4):1287–95.
PMID: 23504926 - Navarro VJ, et al. Liver injury from herbal and dietary supplements. Hepatology. 2017.
PMID: 27677775 - U.S. Food and Drug Administration. FDA Approves First Drug Treatment for Patients with Liver Scarring Due to Fatty Liver Disease. 2024.
fda.gov - American Diabetes Association. Insulin Resistance and Type 2 Diabetes.
diabetes.org - Mayo Clinic. Nonalcoholic fatty liver disease — Symptoms and causes.
mayoclinic.org